Polypharmacy and Prescribing Cascades Drive New Interest in IoT Solutions for Pill Management
Pill Management Systems Represent an Area That Needs to Evolve to Best Serve Elderly Populations and Mitigate Adverse Drug Reactions Among Patients
Life expectancies continue to rise in most parts of the world and so does the rate at which elderly populations are prescribed daily medications and recommended over-the-counter remedies. That should come as no surprise. Historians have suggested that various pills and tablets have been around for at least 3,500 years, dating back to the times when medicinal agents were rolled into balls of honey or dough to maintain consistent dosages and aid in their storage and distribution. The first hand-assembled, gelatin-based pills arrived in the early 1800s, initiating a period of development which, over time, led to the popularity of machine-pressed powder tablets.
At some point along the way, enterprising inventors developed pill boxes to transport and organize these necessities of modern living. Some were purely functional in their design while others trended towards the ornate. These pill boxes evolved from wood to ivory, from jade to copper, from tin to gold, and eventually, to plastic.
Common pill organizers can be found in every corner store today, offering individual compartments to house daily dosages, Sunday through Saturday. The weekly routine of refilling each daily container is expected of its owner. More elaborate electronic designs have been marketed in recent years which add network connectivity and audible alarms to remind patients to take their medicine.
All manner of modern pill box form factors will find a growing market as populations age. The sheer volume of pills pushed on senior citizens is as astounding as it is easy to quantify. The long- and short-term effects of today’s pill-popping culture is a matter of some debate, especially as it relates to aging communities.
According to a 2021 report by healthcare researcher IQVIA, the global medicines market, using invoice price levels, is expected to grow at 3–6% Compound Annual Growth Rate (CAGR) through 2025 to about $1.6 trillion.1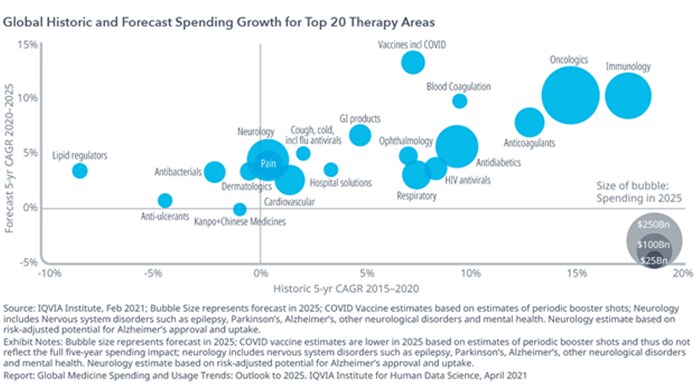
While surveys of daily medication vary by country, the results commonly show expected upticks by age group. It has been ten years since American Nurse magazine suggested that 44% of men and 57% of women older than 65 years take five or more nonprescription and/or prescription medications per week2. A somewhat shocking 12% of persons in this age group were found to take 10 or more nonprescription and/or prescription medications per week. U.S. data from Kaiser Family Foundation (KFF) reported a clear increase in older populations in a 2019 research note. They found that more than half of adults age 65 and older reported taking four or more prescription drugs (54%) compared to one-third of adults age 50–64 years (32%) and about one in ten adults age 30–49 (13%)3.
A Growing Threat: Polypharmacy
Over the last decade, there has been an outcry to remedy the growing problem of polypharmacy, even as the term itself lacks a universal definition. Polypharmacy commonly describes the instances where a person is taking multiple medications to manage multiple ailments. Experts can’t seem to agree on the number of simultaneous prescriptions that would define polypharmacy, but the management of coexisting conditions by multiple healthcare providers often leads to a situation where each patient’s complete medication snapshot is unclear.
It is not unusual for patients with respiratory problems, type 2 diabetes, and existing coronary heart disease to be taking six to nine medications to reduce their long-term risk of further complications and secondary coronary events. In fact, strict adherence to national treatment guidelines for such patients results in a minimum of six concurrent prescription medications. Polypharmacy becomes problematic when negative outcomes occur.
US Pharmacist4
Elderly persons are at a greater risk for Adverse Drug Reactions (ADRs) because of metabolic changes associated with aging and the often-disconnected clinical settings where medicines are prescribed. During 2020, the Covid-19 pandemic contributed a new level of clarity as caregivers from across the healthcare spectrum—hospital clinicians, doctors, telehealth practitioners, primary care physicians, corporate clinicians, nursing home professionals, pharmacists, home care professionals and family caregivers—realized how difficult it was to monitor and dispense medicines during a period of lockdowns. Home delivery of pharmaceuticals from lowest-cost internet sources added an additional disconnect.
Perhaps more troubling is the concept of the prescribing cascade, where the symptoms of an adverse drug reaction are misinterpreted as symptoms of a new ailment, leading to yet another prescription and the potential for negative side effects or unintended drug interactions.
For example, there is perhaps an overabundance of options to treat depression on the market today. Advertisements flood nearly all forms of media in the US: digital, print, radio and television. If a patient is taking a prescribed medication for depression and then seeks medical advice to combat insomnia, an additional prescription may result. Without consideration for the fact that insomnia may be a side effect of the original medication, an adverse reaction of the combined drugs may result. If the insomnia medication is an over-the-counter remedy, healthcare professionals may not even be aware that it has been added to a patient’s daily regimen. Down the road, the patient may complain of light headedness and an attending medical professional may see it as a new condition, unrelated to the pharmaceutical mixture that is the real driver. Now imagine the multiplicity of outcomes when six or medications are taken each day.
The complicated outcomes of polypharmacy can be further exacerbated when patients do not consistently follow their dosing regimens.
IoT and cloud connectivity may already be adding a layer of visibility between patients, their prescriptions and the healthcare providers that manage both.
University Team Introduces an Automated Approach to Pill Management
As longer lifespans push the boundaries of home and telehealth care solutions, pill management systems represent an area that needs to evolve to best serve elderly populations and mitigate adverse drug reactions among patients.
Learn how a student team from the Universitat Politècnica de València (UPV) created an IoT-enabled smart pill dispensing system to automate prescription management.
Microchip and the Internet of Medical Things
As the healthcare industry evolves, the ability to design smart, connected and secure IoT-enabled medical devices is critical. As an experienced medical supplier, we can help you meet these design requirements quickly. We’ve helped medical companies design and manufacture clinical, wearable, implantable and life-critical medical devices for many years. Not only do we have a comprehensive product portfolio, but we lower design barriers with our easy-to-use tools, software and design files. We can also significantly lighten your regulatory burden by providing product with an unmatched history of long product lifecycles to remove the risk of forced redesigns and recertifications, along with our world-class global support and our relentless commitment to quality.
We not only offer reliable parts, but we also provide solutions to address the bigger technology challenges that you face for your next-generation medical device designs.
• Ethernet
• Memory
• Microcontrollers and microprocessors
• Mixed-signal, linear, interface and power solutions
• Touch
• Customized wireless products for implantable and hearable devices
Endnotes
1IQVIA. Global Medicine Spending and Usage Trends: Outlook to 2025. April 28, 2021. www.iqvia.com/insights/the-iqvia-institute/reports/global-medicine-spending-and-usage-trends-outlook-to-2025. Accessed May 10, 2021.
2Preventing Polypharmacy in Older Adults. American Nurse. October 11, 2010. www.myamericannurse.com/preventing-polypharmacy-in-older-adults/. Accessed May 10, 2021.
3Kirzinger, Ashley; Neuman, Tricia; Cubanski, Juliette; Brodie, Mollyann. Data Note: Prescription Drugs and Older Adults. KFF. August 9, 2019. https://www.kff.org/health-reform/issue-brief/data-note-prescription-drugs-and-older-adults. Accessed May 10, 2021.
4Manouchehr Saljoughian, PharmD, PhD. Polypharmacy and Drug Adherence in Elderly Patients. US Pharmacist. July 18, 2019. www.uspharmacist.com/article/polypharmacy-and-drug-adherence-in-elderly-patients. Accessed May 10, 2021.